Researchers continue to find evidence of the strong connection between health factors and the gut microbiome. This connection also occurs in the ‘gut-skin axis’, according to recent research. Dysbiosis between the skin and the gut can contribute to autoimmune skin disorders, acne, psoriasis, and skin inflammation.
Current findings suggest that imbalance in the gut microbiome may be an essential contributing factor in advancing Hidradenitis Suppurativa (HS), an inflammatory skin disease.
The Gut Microbiome and Hidradenitis Suppurativa (HS)
The gut microbiome consists of a wide variety of bacterial organisms. This makeup of microorganisms interacts intricately with other internal body systems and plays a role in defending against environmental pathogens.
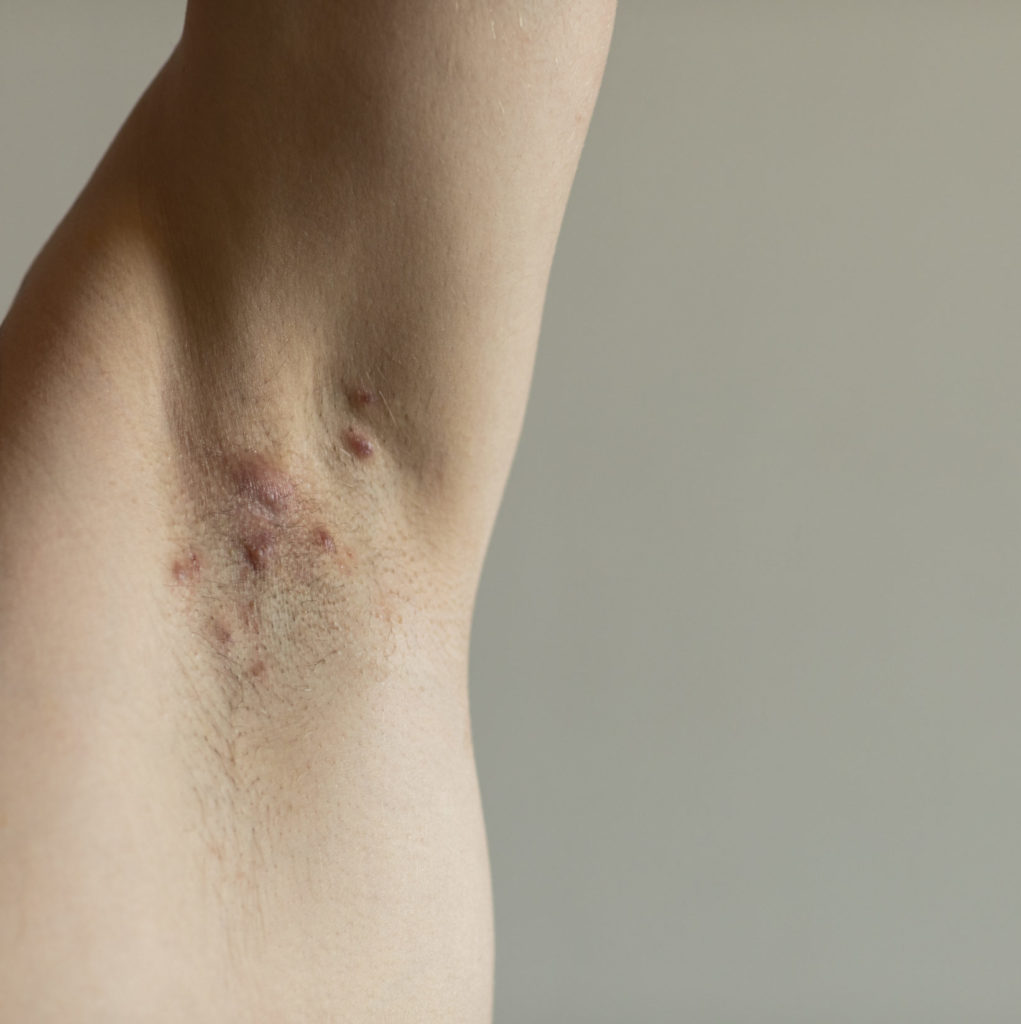
In addition to understanding the gut microbiome, Hidradenitis Suppurativa (HS) is a skin condition that is prone to chronic relapse. The chronic condition has both biological and environmental contributing factors. HS appears as boils and nodules on the skin in gland regions on the body. Currently, HS affects 1-4% of the population, and the condition appears more often in women.
The intricate connection within the “gut-skin axis” prompts researchers to study the intestinal microbiome of HS patients to explore the hypothesis that imbalance in the gut composition may be the underlying culprit of the skin disease.
The Findings
In a recent study, Hacettepe University researchers examined 15 patients with HS and 15 subjects without HS. Each group of participants provided fecal samples for the comparison of microbial content. Findings show significantly lower levels of three types of bacteria (known as Firmicutes), an unclassified type of Clostridiales, an unclassified type of Firmicutes, and Fusicatenibacter in HS patients than in the control group. Lower levels of these bacteria in the gut link to disturbances in the gut flora balance. Also, lower levels of these microorganisms stimulate inflammatory responses through the body.
Future Implications
Additionally, the gut plays a critical part in the development of immune responses. These immune responses stem from specific pathways and from short-chain fatty acids (SCFA) that are products of metabolism. Some bacteria in the gut produce SCFA to balance immune cells that suppress or stimulate inflammatory responses. However, interruptions to this balance, like reduction in this gut bacteria in those with HS, can result in an adverse inflammatory response.
“Our research provides evidence the gut-skin axis is implicated in the progression of this chronic inflammatory skin disorder. While further evidence is required, our research suggests that dietary alteration and personalized probiotic supplementation might also be beneficial for HS patients, particularly since treatment options are limited for these individuals,” explains Dr. Neslihan Demirel Ogut in a statement. Ogut is a doctor at Usak University Training and Research Hospital.
A continuation of the study between the connection of the gut microbiome and HS will be a hopeful aid in future treatment and prevention of this rare skin condition.
This study is presented at EADV 2021 Spring Symposium.
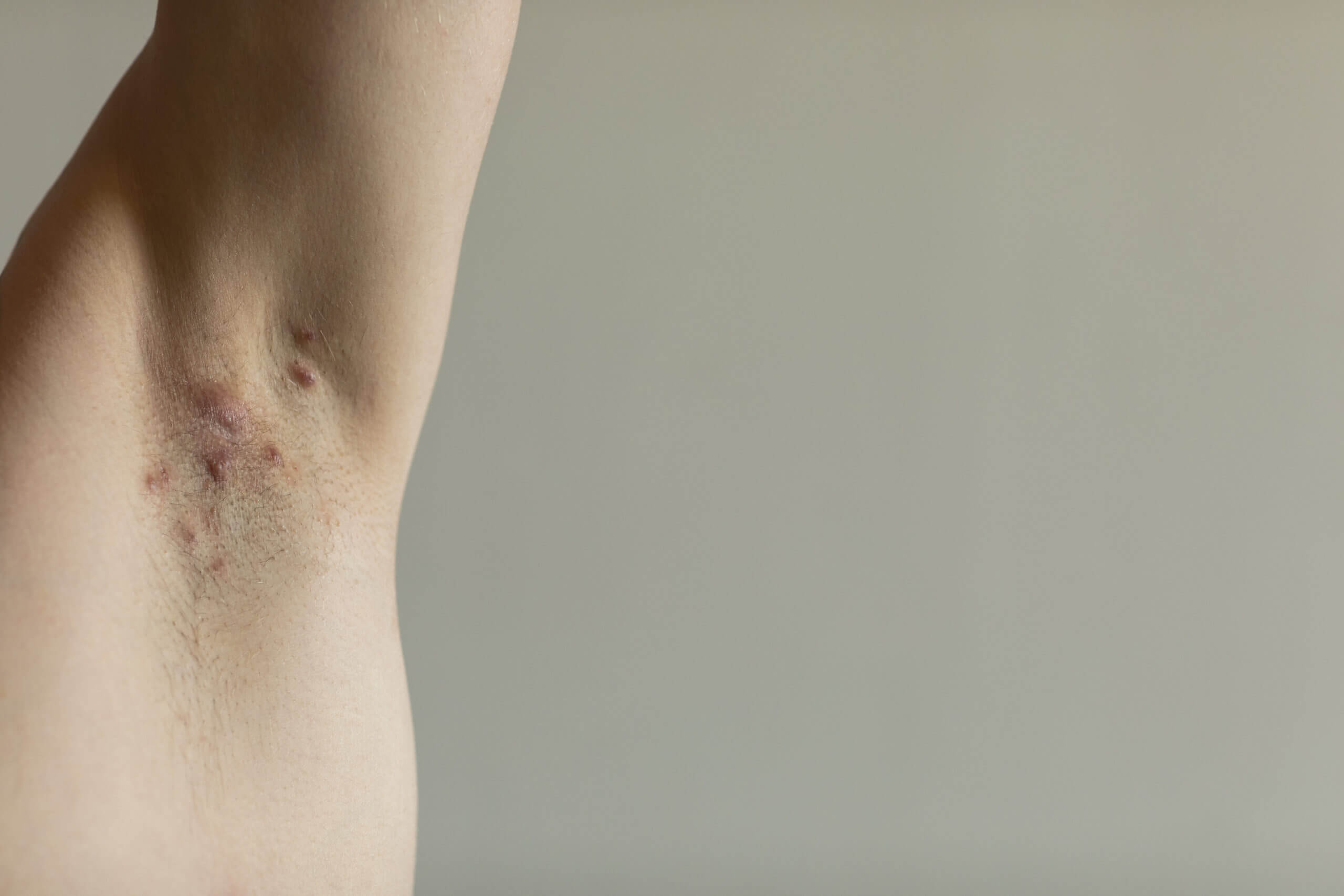
I had this horrific condition in my teens, along with cystic acne. I cleared it entirely by following a mostly-fruit/some vegetable cleansing diet and then fasting on grape juice/lemonade in AM and then a mix of fresh-squeezed beet and carrot blended into tomato-based veg juice in the PM. I eliminated all dairy and meat too, have since returned to including some flesh foods though very sparingly.
Much later in life I recovered from a severe case of chonic “atopic dermatitis” (there are a batch of “doctor don’t know” terms they toss around) by following the science established by Dr. Valter Longo at USC. You can follow him on Youtube or look up his research online. Note NO national media will touch him and fasting is never discussed by the “official” media MDs like Gupta on CNN. Something that is FREE and it WORKS? Not a chance, what would Pfizer and Merck say?